
Cartilage Treatment in Dahisar, Mumbai
Cartilage treatment refers to the repair, restoration, or regeneration of damaged articular cartilage in joints. Articular cartilage is the smooth tissue covering bone ends where they meet to form joints. Once damaged, cartilage has limited capacity to heal because it lacks blood supply. Untreated cartilage injuries progressively worsen and often lead to early osteoarthritis.
Dr. Arpit C Dave, as an experienced Arthroscopic Surgeon in Dahisar, Mumbai, specializes in the full spectrum of cartilage repair including microfracture, OATS, ACI, MACI, and biological treatments like PRP and stem cell therapy. Treatment is selected based on defect size, location, depth, and patient activity level. Early intervention preserves the joint and prevents joint replacement.
What Is an ACL Tear?
Joint pain can come from many sources. Distinguishing cartilage damage from other problems is essential:
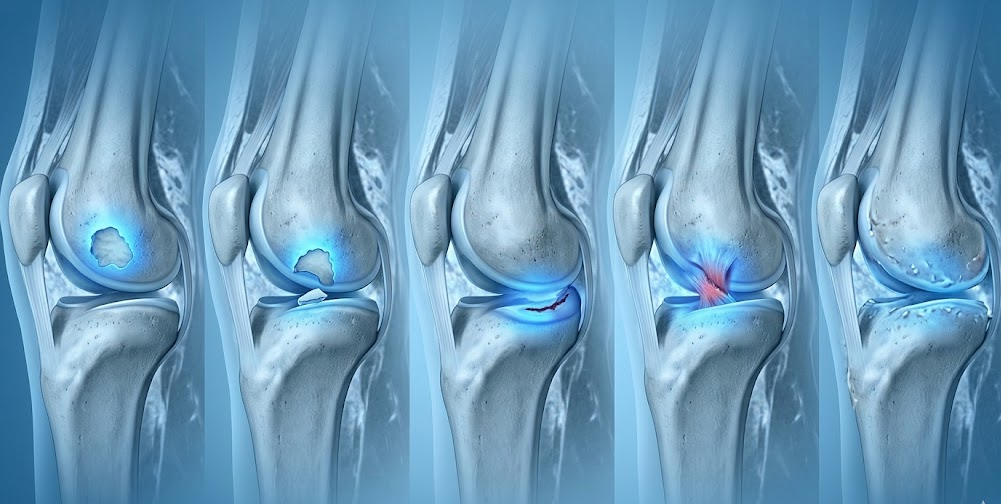
Chondral defect - Pure cartilage damage without bone involvement
Osteochondral lesion - Cartilage damage with underlying bone injury
Meniscal tear - Damage to shock-absorbing cartilage between bones
Ligament injury - Mechanical instability with secondary cartilage stress
Early osteoarthritis - Diffuse cartilage degeneration, not focal injury

Focal cartilage defects are surgically treatable. Diffuse arthritic damage requires different strategies. This distinction completely changes treatment approach.
Acute vs Degenerative Cartilage Damage
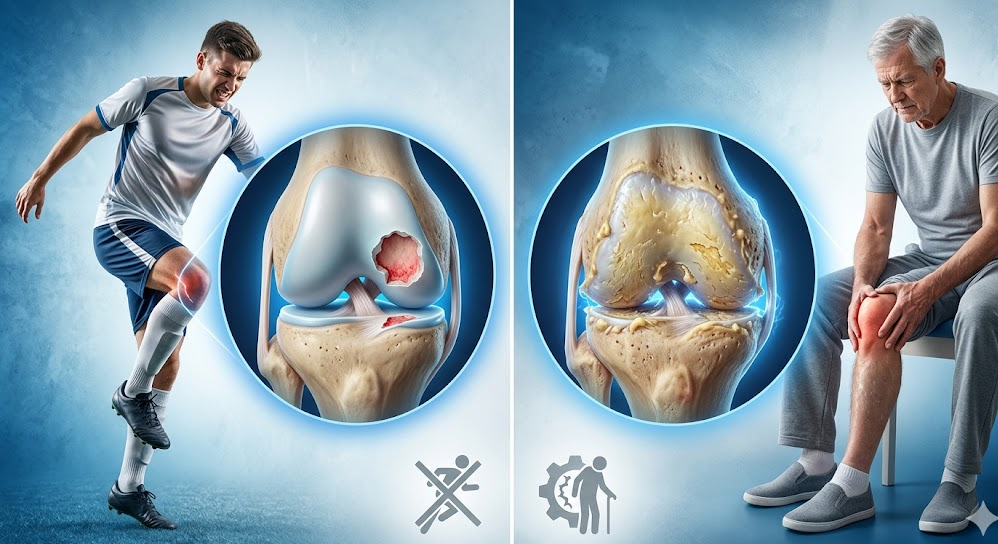
Acute Cartilage Injury
Result of a specific injury, twist, fall, or sports impact. Common in young, active patients. Often associated with ACL tears, meniscal injuries, or patellar dislocations. Damage is well-defined and surrounded by healthy cartilage. These focal chondral defects respond best to repair surgery.

Degenerative Cartilage Damage
Develops gradually from wear and tear, malalignment, obesity, or post-traumatic changes. Damage is diffuse, surrounded by softened, thinning cartilage. Treatment focuses on slowing progression. Advanced cases may require joint replacement.
Why Diagnosis Matters
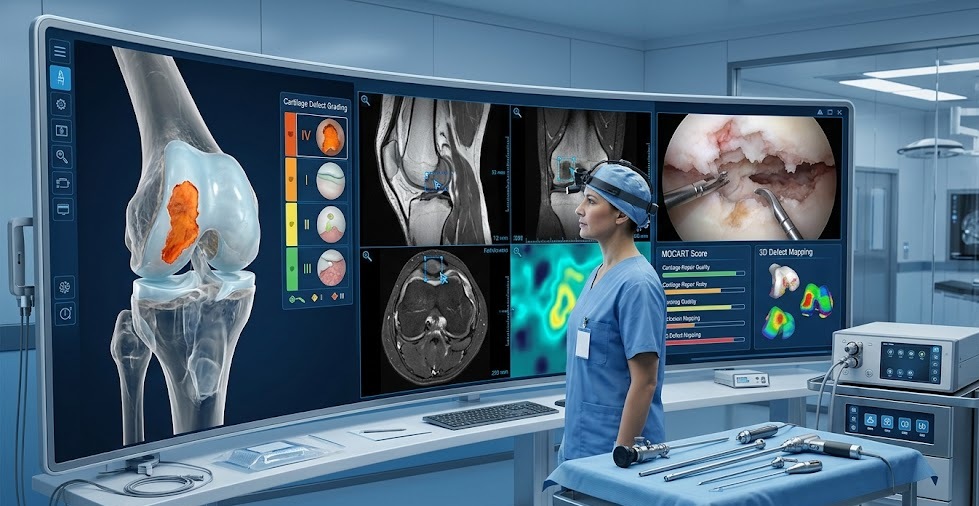
Clinical examination identifies symptoms, but imaging confirms the diagnosis:
X-ray - Shows joint space narrowing, bone changes, alignment
MRI scan - Best test; shows defect size, depth, location, bone marrow edema
CT scan - Useful for osteochondral lesions involving bone
Diagnostic arthroscopy - Direct visualization with simultaneous treatment option

These investigations classify the lesion using Outerbridge or ICRS grading. Grade, size, and depth determine whether you need conservative care, microfracture, transplantation, or cell-based regeneration.
Symptoms You'll Experience
Early Symptoms
Mild, activity-related joint pain that improves with rest. Occasional swelling after exertion. Catching or clicking sensations during movement. Most people ignore these warning signs, allowing the defect to grow.
Progressing Symptoms
Pain becomes frequent and intense. Swelling occurs after routine activities. Locking or giving-way episodes appear when loose cartilage fragments interfere with motion. Stairs and squatting become difficult.
Advanced Symptoms
Persistent pain even at rest. Visible swelling and tenderness. Stiffness limiting daily function. Mechanical locking becomes frequent. At this stage, simple repair may no longer be possible.
Treatment Philosophy - Progressive Approach
Cartilage treatment follows a stepwise progression from biological enhancement to surgical reconstruction. The goal is preserving the natural joint as long as possible.
Stage 1 - Conservative Care & Biological Treatment
Activity modification, weight reduction, and physiotherapy form the foundation. Anti-inflammatory medications manage pain. Viscosupplementation lubricates the joint. PRP delivers growth factors to stimulate healing. Stem cell therapy is offered for select patients. Most small lesions respond well.
Stage 2 - Arthroscopic Debridement
For loose cartilage flaps causing mechanical symptoms, arthroscopic debridement smooths the defect and removes debris. This is a temporizing procedure that improves comfort but does not regenerate cartilage.
Stage 3 - Cartilage Repair Surgery
When biological treatments fail or defects are larger, surgical restoration becomes necessary.
Microfracture Surgery
Arthroscopic procedure for small defects under 2 cm². Tiny holes drilled into subchondral bone allow marrow stem cells to fill the defect, forming fibrocartilage. Quick recovery, minimal cost.
OATS (Osteochondral Autograft Transfer)
Healthy cartilage-bone plugs harvested from non-weight-bearing areas and transplanted into the defect. Restores true hyaline cartilage. Suitable for medium defects (1-4 cm²).
ACI / MACI (Autologous Chondrocyte Implantation)
Two-stage procedure for larger defects. Cartilage cells harvested, cultured for 4-6 weeks, then implanted on a collagen membrane. Best for young patients with large isolated defects.
Osteochondral Allograft
Donor cartilage-bone graft for very large defects. Excellent for complex osteochondral lesions.
Our Cartilage Treatment Procedure
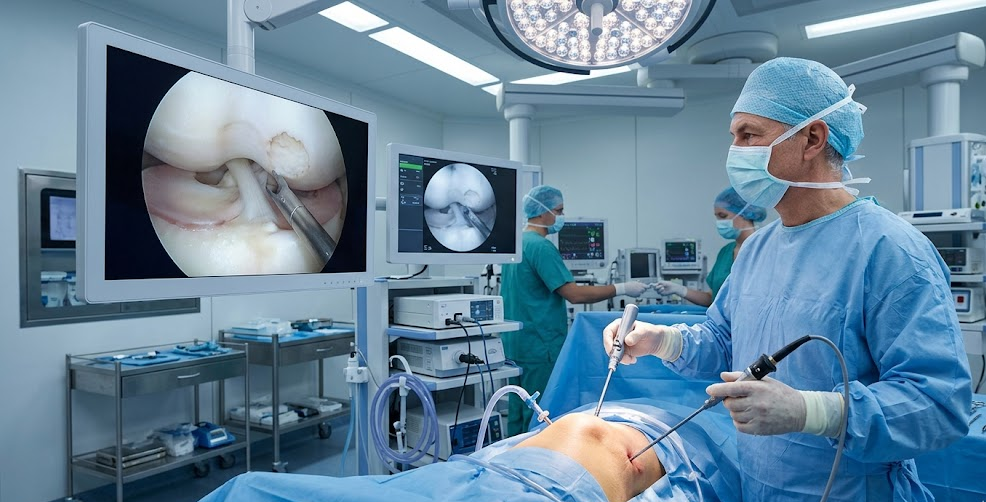
We perform most cartilage repairs arthroscopically through 2-3 small keyhole incisions. Under HD camera visualization, the defect is precisely measured, debrided, and prepared. The selected technique is performed with millimeter precision. Concurrent meniscal tears, ligament injuries, or malalignment are addressed simultaneously. The procedure takes 1 to 3 hours. Most cases go home the same day or after one night.
Chondral defect - Pure cartilage damage without bone involvement
Osteochondral lesion - Cartilage damage with underlying bone injury
Meniscal tear - Damage to shock-absorbing cartilage between bones
Ligament injury - Mechanical instability with secondary cartilage stress
Early osteoarthritis - Diffuse cartilage degeneration, not focal injury

Why Rehabilitation Is Everything
Cartilage repair surgery creates the conditions for healing. The actual healing happens through your post-operative protocol. New cartilage takes 6 to 12 months to mature. Skipping rehabilitation destroys the repair. Your discipline determines outcome more than the surgery itself.
Recovery and Rehabilitation
Recovery Timeline
Week 0 to 2: Protected weight-bearing, ice, gentle motion
Week 2 to 6: Continuous passive motion, progressive range of motion
Week 6 to 12: Gradual weight-bearing, low-impact strengthening
Month 3 to 6: Functional strengthening, swimming, cycling
Month 6 to 12: Sport-specific drills and return to full activity
Rehab Essentials
Strict adherence to weight-bearing restrictions
Continuous passive motion machine when prescribed
Quadriceps and core strengthening for knee cases
Low-impact activities before high-impact return
Avoid running and jumping until cleared
Recovery and Rehabilitation
Cartilage treatment cost in Mumbai varies by technique:
PRP / Stem Cell Injections: ₹15,000 to ₹50,000 per session
Arthroscopic Debridement: ₹80,000 to ₹1.5 lakhs
Microfracture Surgery: ₹1.5 lakhs to ₹2.5 lakhs
OATS Procedure: ₹2 lakhs to ₹3.5 lakhs
ACI / MACI: ₹4 lakhs to ₹8 lakhs
Osteochondral Allograft: ₹3 lakhs to ₹6 lakhs
Costs include surgeon fee, anesthesia, hospital, implants, and post-operative care. Many insurance policies cover surgical cartilage repair.
Why choose Dr. Arpit C Dave?
Dr. Arpit C Dave is an orthopedic and arthroscopic surgeon with over 13 years of practice in joint preservation and cartilage restoration. He approaches cartilage problems diagnosis-first, using MRI assessment with Outerbridge/ICRS grading to classify each lesion and distinguish focal defects from diffuse degeneration. Conservative options like physiotherapy, viscosupplementation, PRP, and stem cell therapy are offered first, with surgery reserved when truly indicated.
When surgery is necessary, Dr. Dave brings international training from Italy, Spain, and France, with expertise across microfracture, OATS, ACI, MACI, and osteochondral allograft transplantation. Concurrent ligament, meniscal, and alignment issues are corrected in the same procedure. He coordinates with sports physiotherapists, prescribes detailed post-op protocols, and conducts return-to-sport testing for athletes in Dahisar, Mumbai.
Frequently Asked Questions
What is articular cartilage and why doesn't it heal?
Articular cartilage is the smooth tissue covering bone ends in joints, allowing frictionless movement. It lacks blood vessels and nerves, so it cannot mount a healing response after injury. Damaged cartilage either stays the same or progressively worsens, which is why active intervention is needed.
How is cartilage damage diagnosed?
MRI is the gold standard, showing defect size, depth, and location precisely. X-rays reveal joint space narrowing in advanced cases. Sometimes diagnostic arthroscopy is needed for direct visualization and grading.
Can cartilage damage be cured without surgery?
Small, early-stage damage can be managed with physiotherapy, viscosupplementation, PRP, or stem cell injections. However, full-thickness defects or larger lesions usually require surgical cartilage repair to restore joint surface integrity.
What is the best cartilage repair surgery?
There is no single best procedure. Microfracture works for defects under 2 cm². OATS suits medium defects. ACI and MACI are preferred for large defects in young patients. Allograft transplantation handles complex lesions. Selection depends on size, depth, location, age, and activity level.
How long does cartilage surgery recovery take?
Initial protected weight-bearing lasts 6 to 8 weeks. Functional recovery takes 3 to 6 months. New cartilage matures over 9 to 12 months. Return to high-impact sports is allowed only after full maturation.
Will I need a knee replacement eventually?
Successful cartilage repair can delay joint replacement by 15 to 25 years or avoid it entirely. The earlier cartilage is treated, the better the long-term joint preservation.
Does PRP regrow cartilage?
PRP does not regrow cartilage strictly, but delivers growth factors that reduce inflammation and may slow progression. PRP works best for early-grade damage and as an adjunct to other treatments.
Can damaged cartilage cause arthritis?
Yes. Untreated cartilage defects increase stress on surrounding cartilage, accelerating wear. The defect grows over time, which is why early cartilage repair is recommended even for moderately symptomatic lesions.
